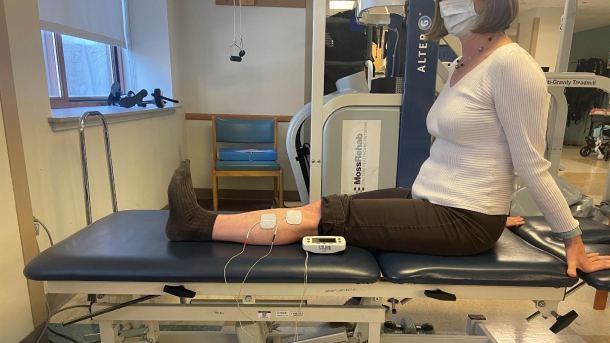
Electrical stimulation is one of the therapeutic tools Jefferson Health has implemented at Jefferson Moss-Magee Rehabilitation Hospital – Elkins Park to help people restore joint and muscle function. It’s the same treatment used in the rehabilitation of actor Jeremy Renner in his recovery from a serious snowplow accident.
After breaking 30 bones in a serious snowplow accident, actor Jeremy Renner received electric stimulation as an element in his rehabilitation. A post in his Instagram story showed how the treatment helped Renner to regain muscle strength and functionality in his leg. Patients at Jefferson Moss-Magee Rehabilitation Hospital – Elkins Park may be in for the celebrity treatment, as therapists utilize this therapeutic intervention in their practices.
Electrical stimulation, or E-Stim, is a non-invasive treatment that sends an electrical current through the skin to stimulate the nerves, thereby contracting the muscles. Electrodes are placed on the skin in the affected area of the body, such as a leg or arm, that receives mild electrical pulses. The end goals may be to relieve pain, strengthen muscles, or retrain movements.
Therapists throughout Jefferson use this intervention as part of their toolbox of treatments to help people improve muscle function or reduce pain after an injury, stroke, or other condition.
“In certain situations, such as after a person experiences a stroke, brain or orthopedic injury, nerves may not fire to the muscle appropriately,” notes Megan Abbott, DPT, supervisor of outpatient therapy at Jefferson Moss-Magee Rehabilitation Hospital – Elkins Park. “E-Stim directed to the muscle can fire all units and maximize muscle contractions to get more strength out of it. E-Stim also helps to retrain those muscles to contract voluntarily.”
Types of Electrical Stimulation
In the same way that medicine is prescribed in different dosages, therapists can utilize varied degrees of electrical stimulation and apply it in diverse ways to meet specific therapy goals. The two most common types of E-Stim include transcutaneous electrical nerve stimulation (TENS) and electrical muscle stimulation (EMS). TENS stimulates the nerves to help lessen pain by interrupting pain signals and releasing endorphins (brain chemicals that relieve pain). TENS, however, does not contract muscles. EMS sends low-frequency electrical impulses to help strengthen and contract muscles. EMS provides greater electrical stimulation intensity than TENS.
“When using electrical stimulation as a pain modulator, TENS therapy can stimulate the surface of the skin and go to pain receptors to help control or reduce pain,” explains Theresa Toczylowski, MPT, clinical manager and physical therapist at Jefferson Moss-Magee Rehabilitation Hospital – Elkins Park. “With EMS, which is intended to produce muscular stimulation, I try to generate movement, improve muscle activation or strengthen the muscle in specific areas of the body.”
Alexey Nastaskin, OTR/L, an occupational therapist who treats patients with neurologic disorders at Jefferson Moss-Magee Rehabilitation Hospital- Elkins Park, uses electromyogram (EMG)-controlled functional electrical stimulation (FES) to facilitate motor learning. Unlike EMS, which stimulates muscles without the person consciously trying to work them, EMG-triggered FES can prompt a person to initiate a voluntary motion. The senses of the successful movement are subsequently reported to the brain. By repeating this process often enough, there is a chance for the brain to relearn “forgotten” movements.
“As an example, if a person is working on improving wrist extension, the electrodes of the FES unit will be connected to wrist extensor muscles,” notes Nastaskin. “A muscle contraction, voluntarily generated by a patient, is assisted at a specific threshold by an electrical stimulation so that the wrist achieves a greater range of motion to promote a functional movement. The application of EMG-triggered FES could be an effective intervention in post stroke hand function recovery in terms of pinching, grasping and releasing.”
Using E-Stim in Therapy
After a knee replacement, ACL (anterior cruciate ligament) knee repair, or other knee surgery, EMS helps quadriceps (front of the thigh) muscles activate to their fullest potential. “After surgery, the body won’t fully activate the quadriceps muscle due to pain”. Patients have a hard time isolating that muscle and figuring out how to recruit it,” says Abbott, who works with outpatients recovering from neurologic and orthopedic conditions. “EMS helps patients realize how that muscle should work by forcing it to contract.”
In cases like Jeremy Renner, who experienced multiple bone fractures and couldn’t activate the muscle on his own, E-Stim would increase the recruitment of nerve units, increase muscle contraction and augment the bulk of muscle. “Our body's reaction to trauma is similar to surgery where the brain is trying to process so much at once,” says Abbott. “From what I see from the video of Renner’s rehabilitation, it looks like E-Stim is used on the quadricep muscle to improve muscle contraction.”
In addition to being implemented when someone is not moving, E-Stim is used in functional training while a person is moving. “We are using E-Stim in our clinic for a person who had a stroke and lost the ability to lift his toes when taking a step. When the front of the foot drags across the floor, it causes tripping and falls,” remarks Toczylowski. “E-Stim helps patients relearn a more normal walking pattern. When the person reaches a certain part of walking, electrical stimulation is activated on the dorsiflexor (the muscle that lifts the foot upward) to clear the foot better. Eventually, the person will start to initiate this movement and hopefully learn to lift the foot on his own.”
During occupational therapy, Nastaskin might use EMG-triggered stimulation to help someone to actively extend the wrist to promote a functional grasp. “Let’s say that a person is able to do a five-degree motion of the wrist but not quite feel it or know if it moved precisely,” notes Nastaskin. “After doing the motion, he receives an electrical stimulation for about five seconds to the particular muscle to help move the joint further up. The EMG-triggered stimulation helps promote neuroplasticity in the brain, which is helping the central nervous system to relearn the movement.”
Nastaskin also uses TENS therapy to relieve chronic and acute pain in an upper extremity. “I may use TENS therapy for a person who has pain in the shoulder muscle due to a variety of conditions,” explains Nastaskin. During rehab, a TENS unit delivers electrical impulses through electrodes placed on the surface of the skin of the shoulder. The E-Stim travels to the brain faster than the pain sensation so the person may perceive the electrical stimulation instead of the pain. “The TENS electrical impulses provide “sensation confusion” by blocking pain channels,” says Nastaskin. “By using TENS therapy, I can slowly train the person’s shoulder to experience normal muscle contraction with reduced pain.”
Best Candidates for E-Stim
When using E-Stim as part of therapy, clinicians initially evaluate its potential benefits – will it help change muscle bulk, activate the muscle to create a movement or reduce pain? “I review a person’s diagnosis and, then, do an evaluation of the patient's muscle strength, how she is walking, and other factors,” explains Abbott. “Based on those evaluations, I may decide to use E-Stim, such as in the situation where the person was dragging the toes when walking.”
A person’s medical and cognitive condition may deter the use of E-Stim therapy. For example, someone with cardiac-related or seizure history, or those with compromised skin integrity, may not be candidates for electrical stimulation. Those with cognitive deficits may not react well to the electrical pulses entering their bodies, as they may not fully understand what is happening.
Others just may find it too uncomfortable and feel they cannot handle the neuromuscular electrical stimulation. “We also don’t use E-Stim on someone with no active muscle movement and whose neurologic system has completely shut off,” notes Abbott. “A person must have some muscle activation.”
While E-Stim devices are commercially available, users should seek medical advice before using one on their own. “I can train people in the clinic on a particular device and order one that they can take home and use it between therapy sessions or after discharge,” explains Nastaskin. “The person can take the device to the clinic during rehab to set it up properly and to ensure the right electrode position and frequency intensity of the electrical system. I also provide recommendations on the amount to use.”
Successful Results
When used as a part of a rehabilitation program, Jefferson clinicians have found E-Stim to be useful for patient recovery. “E-Stim helps during physical therapy after certain knee surgeries to increase the strength in the quadriceps muscle, which is important for stepping up on a stair and getting up and down a seated position,” says Abbott. “It’s the muscle that keeps the leg straight when putting weight on it. If patients feel like their knees are buckling after a knee replacement, the E-Stim can help improve outcomes.”
Toczylowski notes that she has found E-Stim to be successful for patients after ACL repair and as another intervention to help control pain. Nastaskin also says that patients feel empowered as they can see or feel muscles activated to produce a better quality of motion.
“One important question is the longevity of the E-Stim effects,” says Nastaskin. “While we don’t have research-based answer yet, we do see patients improve in the long run.
Discover what Jefferson Moss-Magee Rehabilitation offers in physical therapy.