In our third and final installment of the therapeutic gaming series, we look to the future of gaming therapy by speaking with institute scientists at the Moss Rehabilitation Research Institute about their research on new therapy tools that integrate gaming and virtual reality elements.
As therapeutic gaming proves successful in helping patients get larger and repetitive doses of exercise necessary for recovery, scientists at Moss Rehabilitation Research Institute (MRRI) are taking the lead to develop new gamification applications for use in both the clinic setting and at the patient’s home.
“MRRI scientists are experts in stroke, traumatic brain injury, and Parkinson’s Disease so they understand the neurologic pathways and principles of learning to help develop the most effective gaming therapies,” explains Amanda Rabinowitz, PhD, institute scientist, and director of the Brain Injury Neuropsychology Laboratory at MRRI.
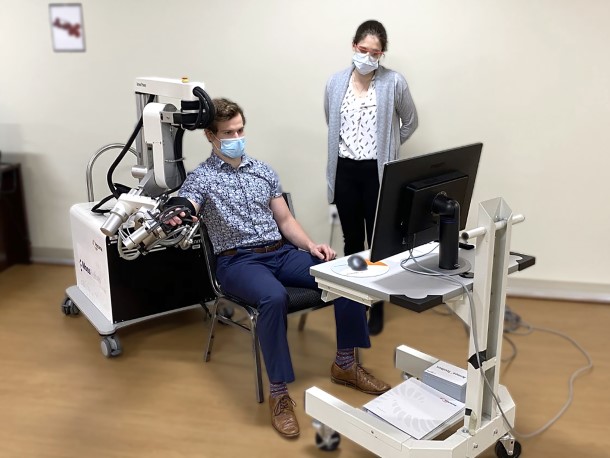
On the forefront is a new therapeutic gaming system for motor recovery after a stroke that uses immersive digital gaming to create an environment in which patients control a dolphin swimming through the water. The study development is led by MRRI Director Dylan Edwards, PhD, together with MRRI Associate Director Laurel Buxbaum, PsyD, MRRI scientists Aaron Wong, PhD, and Shailesh Kantak, PT, PhD, and external investigators Tomoko Kitago, MD, of the Burke Neurological Institute, and John Krakauer, MD, of Johns Hopkins University. This neurosport activity, known as the Mindpod Dolphin from MindMaze, requires patients to move their arms in different interactive activities such as teaching a dolphin to swim, swimming away from sharks, and leaping from the water. The engaging exercises is expected to help people with impaired arm functionality to improve their recovery.
Gaming therapy to reduce phantom limb pain
Another study using virtual reality gamification focuses on reducing phantom limb pain. Dr. Buxbaum, associate director of MRRI, and director of the Cognition and Action Laboratory, is working with MRRI researchers and MossRehab clinicians in collaboration with H. Branch Coslett, MD, Elisabetta Ambron, PhD, and Alex Miller at the University of Pennsylvania on a virtual reality treatment based on the theory of providing alternative feedback to the brain in the form of a visual image of a missing limb. The visual feedback compensates for the missing sensory input that the brain expects when it programs a movement.
During the initial stages of the study, participants with lower-limb amputations performed a series of exercises in the VR lab at MRRI while wearing a VR headset. Activities included scooting around a maze on a virtual chair while kicking down barricades and typing on a virtual keyboard with the legs to surf the Internet. The VR system fills in an image of the missing limb so that amputees see themselves with two complete legs.
“Visualizing and moving limbs simultaneously provides a corrective signal to the brain that reduces phantom limb pain,” explains Dr. Buxbaum. “After completing 5 to 8 sessions, there is a reduction in pain, depression and anxiety that in this study lasts for at least a month.”
The next stage of the study will test a larger group of amputees to confirm initial findings. “We also recently submitted a multi-site National Institute of Health (NIH) grant to develop a home-based version of the intervention so patients can perform therapy remotely,” Dr. Buxbaum remarked.
Virtual reality in neurorehabilitation assessment
Dr. Buxbaum also developed the Virtual Reality Lateralized Attention Test (VR-LAT), an assessment tool that measures the effects of stroke on visual attention, visual search, and multi-tasking. About half of individuals who experience a stroke on the right side of the brain have problems with perception and action on the left side of space. Typically, pencil and paper tests that require patients to bisect lines or cross out specific items on a page are used to diagnose this problem, called spatial neglect. These tests are not sensitive enough to detect subtle deficits and are not strong predictors of performance in the real world.
Wearing a VR headset and using a joystick, individuals performing the VR-LAT travel down a virtual winding path while naming trees and animals and ignoring auditory and visual distractions such as balls rolling across the path or childrens’ laughter. Neglect typically is worse in distracting environments. Using test results, clinicians can determine whether spatial neglect is present and if patients can successfully navigate the real world. The assessment also provides a baseline measurement for therapy.
“The VR-LAT is quick and easy, taking just 10 minutes to administer,” notes Dr. Buxbaum. “It provides a more sensitive assessment of the patient than traditional methods, so the therapist can create an appropriate plan for treatment and discharge from rehab.” MossRehab is the first clinic to implement the test in its Right Hemisphere Stroke Center.
The Virtual Reality Non-Use Test (VR-NU) is another assessment tool developed by Dr. Buxbaum and MRRI research collaborator Dr. Kantak that uses gaming theory to evaluate arm capacity after a stroke. Wearing a VR head-mounted display equipped with headphones and motion tracking controllers affixed to the wrists, study participants reach for objects on different virtual shelves. The VR-NU tracks accuracy, trajectory, and response time in completing tasks under three conditions: easy, hard, or dual task.
“This 10-minute assessment tool will help clinicians diagnose “non-use”, a disabling and common pattern in which individuals use the arm affected by stroke less than they are capable. We will also be able to assess whether non-use occurs more when people are distracted, as is often the case in daily life,” notes Dr. Buxbaum. “We just submitted a National Institute of Health grant proposal to further test this tool before making it available to MossRehab.”
Therapeutic gaming for home therapy
According to Dr. Edwards, about 30% of patients who need neurorehabilitation do not receive therapy due to a lack of transportation and resources. Others who do receive rehabilitation must continue on their own after completing outpatient visits to get better outcomes. Instead of leaving patients with a set of written instructions, home-based therapeutic gaming devices offer more stimulating and visual activities that encourage individuals to exercise harder and longer on their own, and the system can record their performance.
That’s the premise behind the NeuroMotion, a portable gaming console from TRCare, Inc. that assists patients who experienced a stroke in recovering upper extremity functions in their own homes. Dr. Edwards was a principal investigator for a pivotal trial, collaborating with Steven Cramer, MD, at the University of California, Los Angeles (UCLA), where community-dwelling participants performed a series of arm mobility exercises at a gaming workstation. The console features user-friendly buttons and dials and an attachable wand to select and interact with the therapeutic games. Patients can choose from the arcade and computer-based games such as Space Invaders and Whack-a-Mole as well as instructor-led exercise activities. The neurorehabilitation device also features Jeopardy-like cognitive games that ask questions regarding different aspects of patients’ health conditions. Game players receive immediate rewards in their activities while therapists can monitor patient performance and provide feedback in person or via video consultations.
“The telerehabilitation provided by the NeuroMotion is supported by published evidence of its clinical effectiveness for recovery,” notes Dr. Edwards. The next clinical trial of this home-therapy device was recently approved and will be led along with Dr. Alberto Esquenazi, chief medical officer of MossRehab, as a dual-site trial with the pioneering Cramer Laboratory at California Rehab Institute and UCLA.
Investigating mobile rehab applications
Dr. Rabinowitz is working with federally-funded Rehabilitation Engineering Resource Center (RERC) on mobile rehabilitation interventions and therapies for home-based use. Serving as part of a collaborative team of partners from the Shepherd Center, private industry, and the University of California Irvine, Dr. Rabinowitz is examining patterns of engagement with mobile health interventions and designing ways to improve them. As part of this collaboration, Dr. Rabinowitz is leading the development of a chatbot that can carry on personalized interactions with patients to track activities, plans, and goals between therapy sessions, all via text message. Designed to support outpatient brain injury treatment, the chatbot provides encouraging messages, activity updates, and other feedback to help patients meet home therapy goals. A future update may include gamification features that will reward users for progress by enabling them to “level up” and receive virtual rewards to boost therapy effectiveness.
“We also are thinking about adopting a version for use as a self-management tool that walks patients through the process of identifying goals, choosing activities, and making long-term plans,” notes Dr. Rabinowitz.
Another research program is evaluating feedback received from sensor-based neurorehabilitation devices offered by FlintRehab to determine patterns of how people use different gamification features during therapy. Findings will enable developers to design more effective and engaging applications. Dr. Rabinowitz is working to integrate these home-based rehab devices (one is a sensorized glove worn while performing hand and finger exercises to music) with an application called Pt Pal to create a platform that collects data and identifies trends, so clinicians can more closely monitor and determine patient progress between clinical visits.
“Realtime feedback can help clinicians monitor patient progress in between visits,” Rabinowitz remarks. “Data also helps us profile people who remain engaged at a certain functional level to determine the factors that help them get the most from the device. For example, as we found that people who start a session tend to complete it, we can determine that the system is engaging once the user initiates it. We are now working on a reward system to keep people engaged across multiple sessions over days to improve their activity consistency.”
With the help of MossRehab clinicians, MRRI researchers keep their finger on the pulse of therapeutic gaming research and developing new innovative technologies for both in clinic and home-based use. Our goal is to provide our patients and therapists with the best resources to boost the effectiveness of rehabilitation in meeting long-term recovery goals.
Did you miss parts one and two? Read Therapeutic Gaming Part 1: Engaging Patients and Therapeutic Gaming Part 2: Clinical Use now.